Piercing Health · Infection Guide · 2025
Piercing Infection Signs:
Infected vs Irritated — Full Guide
Is your piercing infected — or just irritated? Learn the exact warning signs, how to tell the difference, how to treat it at home, and when to see a doctor immediately.
Medical Disclaimer
This article is for informational purposes only and does not replace medical advice. If you suspect a serious piercing infection — especially involving cartilage, spreading redness, fever, or feeling generally unwell — see a doctor immediately. Cartilage infections in particular can become serious or require hospitalization if not treated promptly.
"Is my piercing infected or just healing?" This is one of the most common — and most anxious — questions in the piercing world. The good news: most piercings that look infected are actually just irritated, and they respond quickly to proper care. But real infections do happen — and knowing the difference can protect both your piercing and your health.
Infected vs Irritated: The Key Distinction
According to piercing industry professionals and medical sources including the Cleveland Clinic and the NHS, in one study as many as 35% of people with pierced ears experienced at least one complication — but the vast majority of those were minor irritation, not true infection.
The critical distinction is this: irritation improves with good aftercare. Infection progressively worsens.
An irritated piercing is caused by physical factors — snagging, pressure, over-cleaning, wrong jewelry, sleeping on the piercing. Remove the irritant and apply proper care, and it resolves. An infected piercing is caused by bacterial invasion of the wound. It requires medical evaluation and often antibiotics — especially if the infection involves cartilage.
The two can look similar in the early stages, which is why so many people panic unnecessarily — or, more dangerously, dismiss a real infection as "just normal healing" for too long.
The single most useful question to ask: Is this getting better day by day — or getting worse? Irritation improves. Infection escalates. If after 2–3 days of proper care your symptoms are worsening rather than improving, take it seriously and see a professional.
What Does Normal Piercing Healing Look Like?
Before you can identify infection, you need to know what normal looks like. Many symptoms that people mistake for infection are simply the normal inflammation and healing response your body has to any wound. According to the NHS and Cleveland Clinic, these are all completely expected in a new piercing:
Normal Healing Symptoms
- Mild redness or slightly darker skin around the piercing site — especially in the first 1–2 weeks
- Slight swelling and puffiness around the piercing immediately after and in the first week
- Tenderness when the piercing is touched or accidentally bumped
- Pale, clear or whitish-yellow discharge — this is lymph fluid, not pus. It dries into "crusties" around the jewelry
- Itching — actually a positive sign that tissue is regenerating
- Small fluid-filled lumps (granulomas) around cartilage piercings — common, not infection
- Slight warmth to the touch in the first few days
The important pattern: these normal symptoms should be mild and improving over time with consistent aftercare. They should not be escalating, spreading, or accompanied by systemic symptoms like fever.
"Crusties" — the dried whitish-yellow crust you find around your jewelry after sleeping — are one of the most misunderstood piercing symptoms. They are completely normal lymph fluid discharge and are actually a sign your body is actively healing. They are NOT pus and NOT infection. Soften them with saline and gently wipe away. Never pick at them dry.
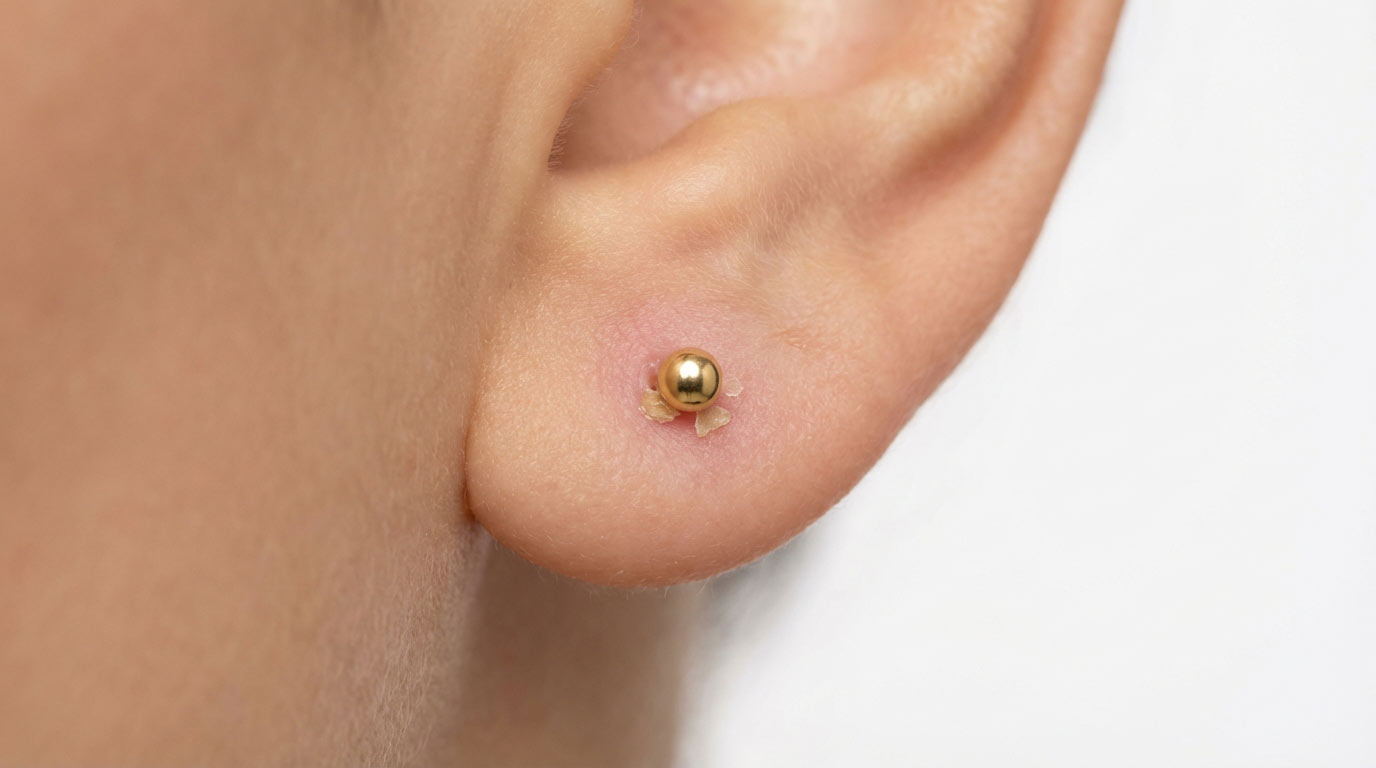
Signs of an Infected Piercing
These are the warning signs that indicate a true piercing infection — not just normal healing or irritation. If you recognize multiple symptoms from this list, see a doctor.
Spreading Redness
Redness that extends beyond the immediate piercing site and continues to expand outward over hours or days. Normal healing redness stays localized right around the piercing hole. Spreading redness is a hallmark sign of an active bacterial infection (cellulitis).
Increasing Swelling & Heat
Swelling that gets progressively worse, not better, over days. The tissue feels noticeably hot and hard. In cartilage piercings, significant swelling can cause the jewelry to become embedded in the tissue — a medical emergency requiring professional removal.
Thick, Discolored, Foul-Smelling Discharge
The clearest indicator of infection: thick, green or dark yellow pus with a distinct, unpleasant odor. Normal discharge is pale yellow-white, thin, and odorless. Infected discharge is thick, often with a strong smell, and accompanies increasing pain rather than decreasing.
Throbbing Pain That Intensifies
Normal healing discomfort decreases over time. An infected piercing produces throbbing, pulsing pain that increases over days rather than improving. Pain that wakes you from sleep or prevents normal movement of the area warrants medical attention.
Fever, Chills, or Feeling Unwell
Systemic symptoms — fever over 100.4°F (38°C), chills, fatigue, sweating, or feeling generally sick — indicate the infection may be spreading beyond the local tissue. This requires immediate medical attention. Do not wait to see if it improves on its own.
Red Streaks Radiating From the Site
Red lines or streaks extending outward from the piercing along the skin are a sign of spreading cellulitis or lymphangitis (infection spreading through lymph channels). This is an emergency — go to urgent care or an ER immediately.
Jewelry Embedding in Tissue
The jewelry clasp, post, or decorative end beginning to sink into or disappear into the skin due to infection-related swelling. Do not attempt to remove it yourself — see a professional piercer or doctor immediately.
Signs of an Irritated Piercing
Irritation is far more common than true infection. According to professional piercers, the majority of "infected-looking" piercings are actually just irritated — and they respond quickly to removing the cause of irritation and improving aftercare.
Common Irritation Symptoms
- Localized redness that doesn't spread beyond the immediate piercing site
- A small raised bump (irritation bump / hypertrophic scar) directly at the edge of the piercing hole
- Mild tenderness that comes and goes — often correlated with specific activities
- Clear or pale yellow discharge (crusties) — normal lymph fluid
- Intermittent itching
- Symptoms that improve when you remove the irritant (stop sleeping on it, remove headphones, switch jewelry)
- Skin redness around where jewelry contacts skin — often a reaction to cleaning products, not infection
Most Common Causes of Irritation

Sleeping on It
Constant pressure from a pillow on a fresh piercing is the #1 cause of irritation bumps. Use a travel pillow.
Headphones/Earbuds
In-ear or over-ear headphones pressing against a healing tragus, helix, or conch piercing cause ongoing mechanical irritation.
Rotating Jewelry
Twisting or spinning jewelry is a persistent myth that actually causes micro-tears and delays healing.
Wrong Products
Alcohol, hydrogen peroxide, or antibacterial soap cause chemical irritation. Use only sterile saline.
Wrong Jewelry Size
Jewelry that hasn't been downsized after initial swelling subsides is too long and snags constantly.
Hair & Clothing
Hair catching on cartilage piercings, tight necklines on chest piercings, waistbands on navel piercings.
Touching Too Much
Unnecessary handling with unwashed hands introduces bacteria and causes both irritation and infection risk.
Over-Cleaning
Cleaning more than twice daily strips the tissue and causes chemical irritation that mimics infection.
Side-by-Side Comparison Chart
Use this comparison to quickly assess your situation:
| Symptom | ✅ Normal Healing | ⚠️ Irritated | 🚨 Infected |
|---|---|---|---|
| Redness | Mild, localized, fading | Localized, comes & goes | Spreading outward, worsening |
| Swelling | Mild, reducing over days | Mild, stable or fluctuating | Increasing, hard, hot |
| Discharge | Clear/pale yellow, odorless | Clear/pale yellow, maybe more | Thick green/yellow, smells |
| Pain | Mild tenderness, improving | Localized, triggers from activity | Throbbing, worsening |
| Heat | Slight warmth, first few days | Mild, localized | Noticeably hot to touch |
| Trend over time | Steadily improving | Improves when irritant removed | Progressively worsening |
| Fever | None | None | Possible — see doctor |
| Action needed | Continue aftercare | Identify & remove irritant | See a doctor |
What Causes Piercing Infections?
According to research published in StatPearls (NCBI), the most common organisms responsible for piercing infections include Staphylococcus aureus, Streptococcus, and Pseudomonas aeruginosa. These bacteria enter the open wound through various routes:
Unwashed Hands
Touching a fresh piercing with unwashed hands is the #1 cause of bacterial introduction. Always wash before touching.
Non-Sterile Equipment
Getting pierced with non-sterile needles or jewelry. Always choose a licensed, professional piercer who uses single-use sterile equipment.
Swimming & Water
Pools (chlorine doesn't kill all pathogens), hot tubs, oceans, and lakes all contain bacteria that can infect a fresh piercing.
Reactive Jewelry
Low-quality, reactive metals (nickel-containing alloys, plated jewelry) cause allergic reactions that damage tissue, opening the door to infection.
Dirty Pillowcases
Pillowcases accumulate bacteria, dead skin cells, and oils quickly. Change them at minimum 2x per week during healing.
Early Jewelry Change
Changing jewelry before a piercing is fully healed reopens the healing channel and introduces bacteria from the new jewelry.
Oral Contact
Kissing, oral sex, or touching oral piercings with unwashed hands are primary infection routes for tongue, lip, and genital piercings.
Wrong Cleaning Products
Hydrogen peroxide, alcohol, and Betadine damage healing tissue and create conditions that allow bacteria to take hold.
According to the Cleveland Clinic, piercing infections don't typically appear immediately — bacteria need 3–7 days to proliferate to symptomatic levels. This means a piercing that looked fine for the first week can still develop an infection in the days following exposure to bacteria.
Piercing Infection Severity Levels
Not all piercing infections are the same. Here's how to assess severity and what to do at each level:
Minor Localized Infection
Slight increase in redness and tenderness, possibly more discharge than usual, no spreading redness, no fever. Usually manageable with improved home care. Monitor closely — if not improving within 3–5 days, see a doctor.
Action: Improve aftercare — sterile saline 3× daily, warm compress, remove irritant. Monitor for 3–5 days.
Established Local Infection
Clear pus discharge (green/yellow), increasing pain and swelling, noticeable heat around the site. Symptoms not improving with home care. See a doctor — may need topical or oral antibiotics. Do not attempt to manage at this level alone.
Action: See a doctor. May require prescription topical or oral antibiotics. Do not treat alone.
Spreading Infection / Systemic Signs
Redness spreading beyond piercing site, red streaks, fever, chills, feeling unwell, or jewelry becoming embedded. This is a medical emergency. Seek urgent care or an emergency room immediately. Cartilage infections at this stage can require IV antibiotics or hospitalization. Do not wait.
Action: Go to urgent care or ER immediately. Do not wait to see if it improves on its own.
How to Treat a Piercing Infection at Home
For minor earlobe infections only. Cartilage infections, spreading infections, or infections with fever must be seen by a doctor.

Critical rule: Do NOT remove your jewelry if your piercing is infected. Removing it allows the piercing hole to close over, trapping the infection inside the tissue and potentially creating an abscess. Leave jewelry in and let discharge drain freely through the open channel. Only remove jewelry on doctor's instruction.
Step 1 — Wash Your Hands Thoroughly
Before touching your piercing at any point during cleaning. Use soap and water. This is non-negotiable.
Step 2 — Clean with Sterile Saline 3× Daily
Gently rinse the piercing with sterile saline wound wash (0.9% sodium chloride) or a salt water solution (¼ tsp non-iodized salt in 8oz distilled water) three times per day during active infection. Do not use alcohol, hydrogen peroxide, or Neosporin — these impede healing and can worsen the situation.
Step 3 — Apply a Warm Compress
Soak a clean paper towel or sterile gauze in warm (not hot) water and hold it gently against the piercing for 5–10 minutes, 3–4 times daily. Warm compresses increase local blood flow, draw out discharge, and help your body fight the infection. This is recommended by the Cleveland Clinic and UPMC for minor infections.
Step 4 — Pat Dry & Leave It Alone
Gently pat dry with clean, disposable gauze or paper towels. Avoid cloth towels. Then leave the piercing alone — no rotating, touching, or disturbing. Monitor closely for improvement.
Step 5 — Monitor Closely for 3–5 Days
A minor infection should show clear improvement within 3–5 days of this regimen. If symptoms are stable or worsening at any point, or you develop fever or spreading redness, stop home treatment and see a doctor immediately.
When to See a Doctor — Non-Negotiable Signs
See a doctor immediately if you have ANY of these:
- Redness spreading beyond the immediate piercing area and continuing to expand
- Fever above 100.4°F (38°C), chills, or feeling generally unwell
- Red streaks radiating outward from the piercing — possible lymphangitis (medical emergency)
- Jewelry appears embedded in the tissue or is sinking into the skin
- The piercing involves cartilage and shows any signs of infection — cartilage infections are medically serious
- Symptoms not improving after 3–5 days of proper home care
- Thick green or yellow pus that is increasing in amount
- Swelling severe enough that the jewelry is under pressure against the skin
What the Doctor May Do
According to the Cleveland Clinic and NHS, medical treatment for piercing infections may include:
- Topical antibiotic ointment for mild surface infections
- Oral antibiotics (typically covering Staphylococcus) for established infections
- IV antibiotics or hospitalization for serious cartilage infections (perichondritis)
- Incision and drainage if an abscess has formed
- Assessment of whether jewelry should be left in or removed — the doctor will advise based on the severity
Note: Many GPs and ER doctors are not specialized in piercing care. If possible, see an ENT (ear, nose, throat) specialist or a dermatologist for ear piercings. If the infection isn't responding to prescribed antibiotics within the expected timeframe, follow up and ask if a culture was taken to identify the specific bacteria.
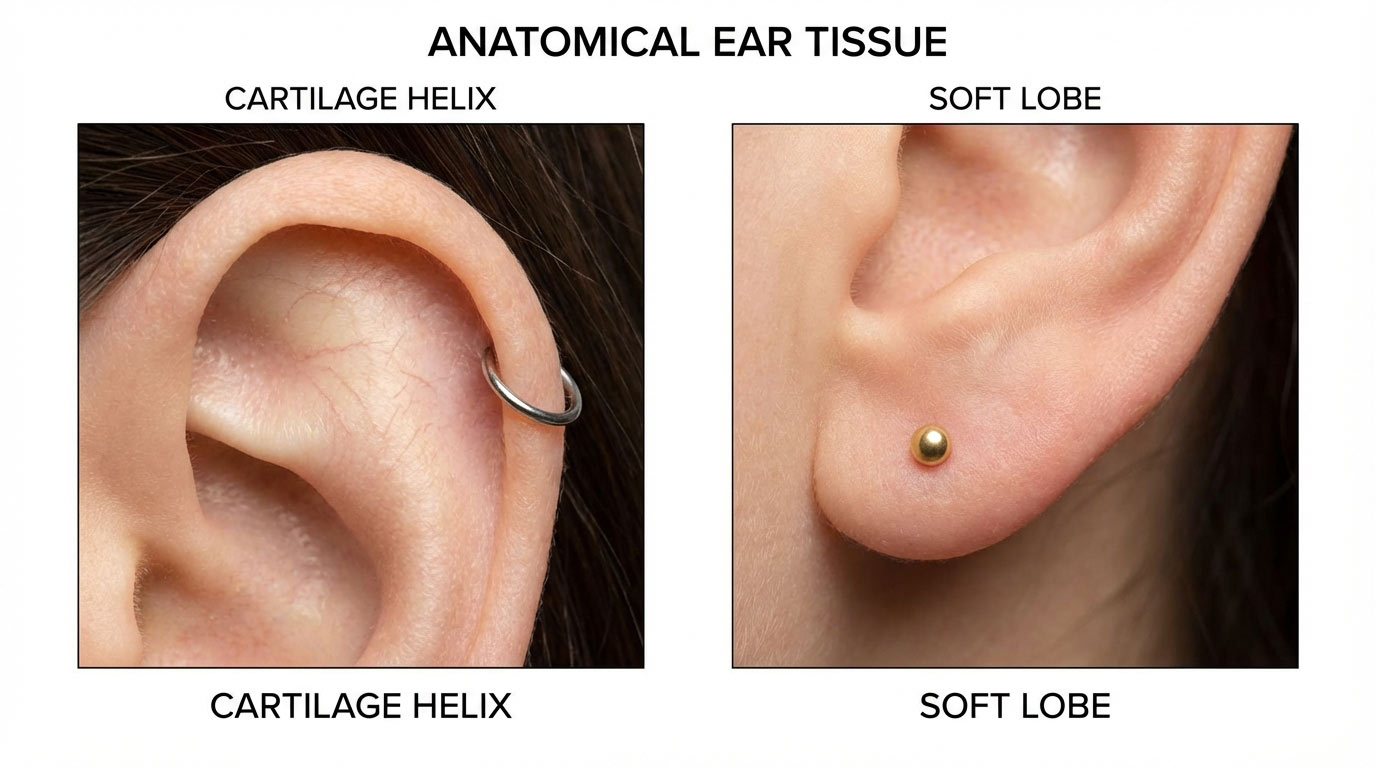
Cartilage vs Lobe: Why It Matters So Much

The distinction between a lobe piercing infection and a cartilage piercing infection is not a minor one. According to both Healthline (medically reviewed) and the Cleveland Clinic:
Earlobe Infections
Earlobe tissue is fleshy with strong blood supply. Minor infections are generally manageable at home if caught early. Most clear up within a week of proper care. Still monitor closely and see a doctor if not improving.
Cartilage Infections
Cartilage has very limited blood supply, so antibiotics reach it poorly. Infections spread through cartilage rapidly and can cause perichondritis — a severe infection of the cartilage membrane that can permanently deform the ear. These must be treated by a doctor promptly. Many require oral antibiotics; severe cases need IV antibiotics or hospitalization.
Cartilage Infection Warning
If you have a cartilage piercing (helix, tragus, daith, rook, conch, industrial) and notice any of the infection signs listed above — particularly spreading redness, increasing pain, or fever — do not attempt home treatment. See a doctor the same day. Cartilage infections can go from manageable to serious in 24–48 hours.
How to Prevent Piercing Infections
DO
- Choose a licensed, professional piercer who uses single-use sterile needles and autoclave-sterilized equipment
- Request implant-grade jewelry — titanium (ASTM F136), 14k+ solid gold, or implant-grade steel
- Clean twice daily with sterile saline wound wash for the entire healing period
- Change pillowcases at minimum twice per week
- Wash hands thoroughly before every touch of your piercing
- Return to your piercer for a downsizing appointment 4–6 weeks after the initial piercing
- Rinse mouth with alcohol-free mouthwash after meals for oral piercings
DON'T
- Never pierce yourself or allow an unlicensed person to pierce you — risk of infection is dramatically higher
- Don't touch your piercing with unwashed hands — ever
- Don't swim in pools, hot tubs, oceans, or lakes for the duration of healing
- Don't use alcohol, hydrogen peroxide, Betadine, or antibacterial soaps
- Don't rotate or twist your jewelry — this is one of the most common infection-causing mistakes
- Don't change your jewelry early — especially before full healing is confirmed by your piercer
- Don't use piercing guns — they cannot be fully sterilized and cause more trauma to tissue than needles
Frequently Asked Questions
What are the signs of an infected piercing?
Signs of an infected piercing include: spreading redness beyond the piercing site, increasing swelling and heat, thick green or yellow discharge with a foul smell, throbbing pain that worsens over time, fever or chills, and red streaks radiating from the site. Normal healing involves mild redness and clear/whitish discharge that improves with aftercare — infection involves symptoms that progressively worsen.
How do I know if my piercing is infected or just irritated?
The key difference: irritation improves; infection worsens. Irritated piercings have localized redness, mild tenderness, and clear/pale discharge that get better when you remove the irritant (pressure, snagging, wrong products) and improve aftercare. Infected piercings have symptoms that escalate — spreading redness, thickening discharge, increasing pain, possible fever — regardless of care.
Should I remove my jewelry if my piercing is infected?
No — do not remove your jewelry unless a doctor specifically instructs you to. Removing the jewelry allows the piercing hole to close over, trapping the infection inside the tissue and potentially forming an abscess. The jewelry acts as an open channel for infected discharge to drain. Leave it in and see a medical professional.
Can I treat a piercing infection at home?
Minor earlobe infections can sometimes be managed at home: clean with sterile saline 3x daily, apply warm compresses, monitor closely. However, cartilage infections must be seen by a doctor — they are significantly more serious and can become severe quickly. Any infection with fever, spreading redness, or not improving after 3–5 days of home care requires medical attention.
What does infected discharge look like vs normal discharge?
Normal discharge is clear to pale whitish-yellow, thin, odorless or very mild smell, and dries into "crusties" around the jewelry. Infected discharge (pus) is thick, opaque, green or dark yellow in color, often with a distinct unpleasant odor, and is accompanied by increasing pain and redness rather than decreasing symptoms.
Can an old healed piercing get infected?
Yes — even fully healed piercings can become infected, although it's less common. This can happen from wearing jewelry with reactive metals, poor hygiene when changing jewelry, a traumatic snagging injury that reopens the tissue, or exposure to bacteria through dirty jewelry or hands. The treatment approach is the same as for new piercing infections.
Will an infected piercing close up if I leave the jewelry in?
An infected piercing is unlikely to close up while the jewelry is in and infection is active — the inflammation actually keeps the channel open. The risk of closure comes if you remove the jewelry, which is why medical guidance is to keep it in during treatment. Once the infection fully clears, your piercer can advise on whether the piercing channel remains viable.
Related Reading
Have questions about your piercing's symptoms?
Drop them in the comments — we answer every one!
